Негритянка с огромной жопой и сочными дойками Даллас Плейхаус ведет себя слишком уверено перед своим супругом. Все дело в том, […]
Красивая эротика с обнаженными топ-моделями на сайте Рукоеб в HD качестве.

Соблазнила незнакомца в гараже и была жестко выебана
Темноволосая девка увидела, что мужик чинит ее машину в гараже и захотела отблагодарить его сексом. Привлекательная цыпочка соблазнила незнакомца и […]

Татуированную красотку жестко поимели в мокрую письку
Симпатичная татуированная брюнетка Bambi Silk (Бамби Силк) отлично проводит время со своим приятелем, у которого реально здоровенный фаллос. Телочка раздвигает […]

Полнометражная порно пародия на Могучих Рейнджеров с Кимми Грейнджер
Действие полнометражной порно пародии на Могучих Рейнджеров разворачивается вокруг симпатичной скромницы Кимми Грейнджер. Эта скромная милашка на самом деле скрывает […]

Репетиторша присоединилась к студентке и её бойфренду в групповухе
Зрелая блондинка преподавала репетиторское занятие молодой студентке, когда пришел её возбужденный бойфренд. Парню очень хотелось секса, поэтому он тут же […]

Брюнетка громко кончает от хардкорного секса
Сексуальная брюнетка лежит на диване с кляпом во рту, поэтому ее громкие стоны слышны всем вокруг. Девушке нравится подчиняться своему […]

Хардкорный анальный трах с татуированной блондинкой в колготках
Красивая татуированная блондинка собирается как следует порезвиться со своим новым ухажером и для этого надевает самое эротичное нижнее белье с […]

Трахнул девушку с огромной задницей прямо на дороге
Рыжеволосая красотка каталась на велосипеде, как вдруг ее задница застряла между машинами. Чтобы освободиться, она позвала на помощь первого попавшегося […]

Похотливая секретарша страстно ебется с боссом на рабочем столе
Возбужденная блондинка соблазняет зрелого босса, раздвигая перед ним ноги на рабочем столе. Опытный мужик пристраивается к похотливой секретарше сзади и […]

Грудастая латинка подставляет попку для ебли после тренировки
Темноволосая латинка Канела отлично провела свою тренировку и вернулась домой в кружевном нижнем белье и в сетчатых чулках. Этого оказалось […]

Красотка с короткой стрижкой раздвигает ноги для бурного секса
Толстая красотка с короткой стрижкой возбуждает мужика одним своим видом, ведь ее огромные сиськи так и тянутся в ладони, а […]

Похотливая мачеха кончает от секса с пасынком
Похотливая блондинка лежала в постели и страстно мастурбировала свою мокрую пизденку, когда в комнату вошел ее пасынок. Чувак заметил все […]

Милфа соблазнила молодую няню и устроила лесбийский секс
Сексапильная милфа вернулась домой раньше обычного и застала свою молодую няню за просмотром порно на кухне. Женщина была так возбуждена […]

Жаркий секс негритянки с брутальным полицейским за контрабанд
Молодая негритянка попалась с контрабандой, поэтому теперь сидит в наручниках в комнате у брутального полицейского. Чернокожая цыпочка просит отпустить ее […]
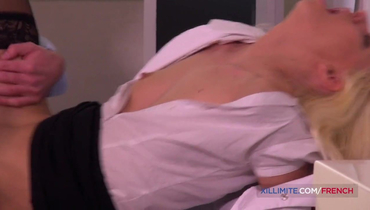
Анальный трах после минетной анестезии на стоматологическом кресле
Длинноволосая блондинка разделась до нижнего белья перед приемом стоматологом, даже не догадываясь о том, что ее ждет сюрприз. Стоматолог вместе […]

Жена негритянка шпилится с черным любовником на глазах у мужа куколда
Негритянка с большими силиконовыми сиськами завела себе чернокожего любовника, с которым часто изменяет своему мужу. Куколд даже не пытается что-то […]

Сисястая мамка друга страстно ебется с пацаном в общаге
Возбужденная брюнетка приходит в гости к лучшему другу своего сына. Молодой парень и представить себе не мог, что грудастая мамка […]

Блондинка СлимТик Вик трахается с негром пока разговаривает по телефону с мужем
Горячая блондинка СлимТик Вик общается по телефону со своим мужем, рассказывая ему о том, как сексуально она сегодня чувствует. На […]

Чтобы получить роль, Анне Полине пришлось заняться сексом с продюсером
Длинноволосая красотка Анна Полина готова на многое, лишь бы получить главную роль в новом фильме. Придя к продюсеру на собеседование, […]

Застукала сына за трахом с блондинкой и предложила секс втроем
Жопастая мамка вернулась домой раньше, чем должна была и застукала своего сына за страстным сексом с горячей блондинкой в короткой […]

Молодая блондинка ебется с отчимом в костюме Фреда Флинстоуна
Сексуальная молодая блондинка переоделась в костюм Фреда Флинстоуна и собиралась заняться лесбийским сексом с подругой. Но зрелый опытный отчим не […]

Голая блондинка мерит трусики в примерочной на скрытую камеру
Красивая девушка заходит в примерочную магазина нижнего белья, не подозревая, что в этом магазине установлены скрытые камеры, снимающие стройную голую […]

Любительский анальный секс молодой пары с окончанием внутрь
Эта парочка прекрасно проводит время вместе. Сегодня у них запланирован жесткий анальный секс, о котором они давно уже мечтают. Милашка […]

Кэнди Лишес и Зази развели сводного брата на секс втроем
Похотливые подружки Кэнди Лишес и Зази прокрались в дом, где жил их сводный брат Алекс, с единственной целью — соблазнить […]

Парень жестко выебал в глотку девушку в черных чулках
Стройная девушка в черных чулках становится на колени перед бойфрендом и отправляется с ним в спальню, ведь там будет жаркая […]

Развратные мамки занимаются лесбийским сексом в позе 69 пока их сыновья не замечают
Молодые сыновья весело проводили время вместе, играя в приставку, даже не подозревая о том, чем в это время занимаются их […]
